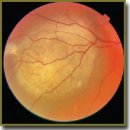
The Role of Pathologic and Molecular Genetic Factors in Development of Uveal Melanoma Extrabulbar Growth
The aim of the investigation is the disclosure of tumor extrabulbar growth association with pathologic and molecular genetic changes in patients with uveal melanoma.
Materials and Methods. 134 patients with uveal melanoma at the age of 22 to 84 years were examined and treated. The average height of the tumor was 9.2±2.9 mm, basal diameter was 15.3±3.5 mm. In 97.8% of cases enucleation of the affected eye was performed. Histological tumor types were spindle cell (n=61; 45.6%), mixed (n=46; 34.3%), and epithelioid (n=27; 20.1%). Using the PCR–RFLP analysis (polymerase chain reaction–restriction fragment length polymorphism) and deletion mapping method were determined full and partial monosomy of chromosome 3, deletions of the short arm of chromosome 1 and RASSF1A gene methylation (n=134). The patients were divided into two groups: the presence (n=15) and the absence (n=119) of extrabulbar growth.
Results. Significantly lower rate (20 vs. 47.9%) of spindle cell type spindle cell type in the group with extrabulbar growth is shown. The frequency of full or partial monosomy of chromosome 3 in the group with extrabulbar tumor growth was significantly higher (80 vs. 50.4%). When comparing the groups on age and sex of the patient, the height and basal diameter, ciliary body involvement, tumor pigmentation, the presence of hemophthalmia, retinal detachment, subretinal exudate, family history, deletion of the short arm of chromosome 1 and the RASSF1A gene methylation no significant differences were found.
Conclusion. A statistically significant number of patients with uveal melanoma showed favorable tumor prognosis in the spindle cell tumor type and negative prognosis when detecting monosomy of chromosome 3, which correlated with the extrabulbar tumor growth. To determine the relationship between the probability of extrabulbar tumor growth and other molecular genetic changes in further researches are needed.
- Brovkina A.F. Oftal’moonkologiya [Ophthalmic oncology]. Moscow: Meditsina; 2002; 424 p.
- Saakyan S.V., Amiryan A.G., Tsygankov A.Yu. Uveal melanoma in the children and adolescents: the analysis of the original observations of 21 patients. Rossiiskaya pediatricheskaya oftal’mologiya 2015; 10(3): 33–36.
- Saakyan S.V., Amiryan A.G., Tsygankov A.Yu., Sklyarova N.V., Zaletaev D.V. Clinical, pathomorphological and molecular genetic aspects of uveal melanoma with highmetastatic risk. Rossiyskiy oftal’mologicheskiy zhurnal2015; 8(2): 47–52.
- Brovkina A.F. Differential diagnosis of choroidal melanoma. Oftal’mologicheskie vedomosti 2008; 4(1): 68–76.
- Shields C.L., Furuta M., Berman E.L., Zahler J.D., Hoberman D.M., Dinh D.H., Mashayekhi A., Shields J.A. Choroidal nevus transformation into melanoma: analysis of 2514 consecutive cases. Arch Ophthalmol 2009; 127(8): 981–987, http://dx.doi.org/10.1001/archophthalmol.2009.151.
- Amiryan A.G., Saakyan S.V., Valsky V.V. Extraocular extension of uveal melanoma after organ-preserving treatment. Rossiyskiy oftal’mologicheskiy zhurnal 2011; 4(3): 15–19.
- Neroev V.V., Saakyan S.V., Amiryan A.G., Valsky V.V. Risk factors of extraocular spread after local treatment of uveal melanoma. Vestnik oftal’mologii 2011; 2: 21–25.
- Saakyan S.V., Tsygankov A.Iu., Amiryan A.G., Skljarova N.V., Zaletaev D.V. Role of molecular and genetic factors in survival from uveal melanoma. Vestnik oftal'mologii 2016; 132(1): 3–9.
- Damato B., Coupland S.E. A reappraisal of the significance of largest basal diameter of posterior uveal melanoma. Eye (Lond) 2009; 23: 2152–2160.
- Tsygankov A.Yu., Saakyan S.V., Amiryan A.G. The role of molecular genetic factors in survival of ciliochoroidal uveal melanoma patients. Meditsinskiy vestnik Bashkortostana 2014; 9(2): 147–150.
- Weis E., Shah C.P., Lajous M., Shields J.A., Shields C.L. The association between host susceptibility factors and uveal melanoma: a meta-analysis. Arch Ophthalmol 2006; 124: 54–60, http://dx.doi.org/10.1001/archopht.124.1.54.
- Frenkel S., Zloto O., Pe’er J., Barak V. Insulin-like growth factor-1 as a predictive biomarker for metastatic uveal melanoma in humans. Invest Ophthalmol Vis Sci 2013; 54(1): 490–493, http://dx.doi.org/10.1167/iovs.12-10228.
- el Filali M., Missotten G.S., Maat W., Ly L.V., Luyten G.P., van der Velden P.A., Jager M.J. Regulation of VEGF-A in uveal melanoma. Invest Ophthalmol Vis Sci 2010; 51(5): 2329–2337, http://dx.doi.org/10.1167/iovs.09-4739.
- Mallikarjuna K., Pushparaj V., Biswas J., Krishnakumar S. Expression of epidermal growth factor receptor, ezrin, hepatocute growth factor, and c-Met in uveal melanoma: an immunohistochemical study. Curr Eye Res 2007; 32(3): 281–290, http://dx.doi.org/10.1080/02713680601161220.
- Pinzani P., Mazzini C., Salvianti F., Massi D., Grifoni R., Paoletti C., Ucci F., Molinara E., Orlando C., Pazzagli M., Neri B. Tyrosinase mRNA levels in the blood of uveal melanoma patients: correlation with the number of circulating tumor cells and tumor progression. Melanoma Res 2010; 20(4): 303–310, http://dx.doi.org/10.1097/cmr.0b013e32833906e3.
- Saakyan S.V., Amiryan A.G., Tsygankov A.Yu., Loginov V.I., Burdennyy A.M. Mutations in oncogenes GNAQ and GNA11 in uveal melanoma patients. Molekulyarnaya meditsina 2014; 2: 34–37.
- Saakian S.V., Amirian A.G., Tsygankov A.Yu., Loginov V.I., Burdenny A.M. Association of the ABCB1 gene with risk for uveal melanoma. Arkhiv patologii 2014; 76(2): 3–7.
- Prescher G., Bornfeld N., Hirche H., Horsthemke B., Jockel K.H., Becher R. Prognostic implications of monosomy 3 in uveal melanoma. Lancet 1996; 347(9010): 1222–1225, http://dx.doi.org/10.1016/s0140-6736(96)90736-9.
- Worley L.A., Onken M.D., Person E., Robirds D., Branson J., Char D.H., Perry A., Harbour J.W. Transcriptomic versus chromosomal prognostic markers and clinical outcome in uveal melanoma. Clin Cancer Res 2007; 13(5): 1466–1471, http://dx.doi.org/10.1158/1078-0432.ccr-06-2401.
- Van Raamsdonk C.D., Griewank K.G., Crosby M.B., Garrido M.C., Vemula S., Wiesner T., Obenauf A.C., Wackernagel W., Green G., Bouvier N., Sozen M.M., Baimukanova G., Roy R., Heguy A., Dolgalev I., Khanin R., Busam K., Speicher M.R., O’Brien J., Bastian B.C. Mutations in GNA11 in uveal melanoma. N Engl J Med 2010; 363(23): 2191–2199, http://dx.doi.org/10.1056/nejmoa1000584.










