Modern Technologies of Bronchial Asthma Control in Children (Review)
Bronchial asthma ranks among the most common allergic diseases in children. It is chronic inflammatory disease of the respiratory tract, in which many cells of innate and adaptive immune system participate together with epithelial cells causing the main clinical syndromes typical for the disease. Currently, bronchial asthma therapy aims at obtaining the control over the symptoms and course of asthma by providing an anti-inflammatory baseline therapy using different groups of pharmaceuticals: inhaled glucocorticosteroids, leukotriene receptor antagonists, cromones, beta-2-agonists and long-acting theophyllines, systemic glucocorticosteroids and anti-IgE-therapy. However, despite a wide range of approaches to anti-inflammatory baseline therapy, it is still a problem to obtain the disease control in most patients indicating the necessity for searching new therapeutic approaches. In this regard, to optimize pathogenetic therapy of bronchial asthma, the work is being currently carried out to improve the existing anti-inflammatory drugs and their combinations. Moreover, there is a search for crucially new approaches to asthma treatment with due consideration of the disease phenotypes and endotypes including development and practical application of pharmaceutical drugs with anti-cytokine and anti-mediator effects. Probably, as far as the knowledge of molecular characteristics of asthma endotypes is being refined, and there being introduced the biomarkers enabling to diagnose asthma phenotypes and endotypes and monitor asthma control, there will be implemented an individual approach in individual therapy administration.
According to epidemiological studies, 5–10% children suffer from bronchial asthma (BA) [1]. BA is chronic inflammatory disease of the respiratory tract, in which many cells of innate and adaptive immune system in combination with epithelial cells are involved causing the main clinical syndromes typical for the disease [2, 3]. BA is thought to be heterogeneous. Different phenotypes and endotypes of the disease have been distinguished, they are specified by the interaction of genetic and environmental factors and differ in age of the disease, clinical presentations, the range of biomarkers, prognosis and response to conventional and novel therapeutic treatment [4–7]. However, asthma phenotypes diagnosed considering certain inflammatory cell populations prevailing in sputum have been shown to be unstable during a 12-month follow up period [8].
Immunologic mechanisms underlying BA are mediated primarily by Т-helper cells type 2 (Th2) associated with immunoglobulin E hyperproduction and the formation of eosinophilic type of respiratory inflammation [2]. However, some aspects of eosinophilic inflammation can be associated with the activation of innate lymphoid cells type 2 (ILC-2), which act in combination with basophilic cells [9]. Moreover, some BA phenotypes are characterized primarily by neutrophillic inflammation controlled by the subsets of Th17 helper Т-cells [10–12].
In most children BA formation is associated with Th2-variant of an immune response, atopy, innate tendency for hyperproduction of total and specific IgE, reduced functional activity of T-reg-cells (Тh3, Tr1, CD4+, CD25+) and Th1/Th2 imbalance [4, 13–16]. The interaction of specific IgE with causally significant allergens on the surface of mast cells and basophils induces the release of preformed and synthesized de novo mediators causing acute inflammation of bronchi accompanied by cell migration in respiratory mucosa and formation of cell infiltrate including eosinophils, basophils, Th2-lymphocytes with the involvement of macrophages, monocytes, dendritic, mast and epithelial cells, platelets, neutrophils, fibroblasts [17]. Pro-inflammatory cytokines released by mast cells, eosinophils, basophils, Th2-lymphocytes contribute to chronic inflammation development. Pro-inflammatory cells migrate from blood stream into intercellular space under the influence of chemokines and adhesive molecules [2].
Allergic inflammation persistence in the respiratory tract is promoted in BA by long exposure to causally significant allergens, the presence of high atopy index in a patient, the release of inflammatory neurokinins (substance Р, neurokinins А and В) by nerve cells, and associated viral, bacterial or atypical (chlamydial, mycoplasmal) infections [18–22].
Since asthma is characterized by recurrent variable respiratory obstruction, the disease control can be assessed relying on the intensity of its symptoms, external respiration parameters, the findings of functional tests showing bronchial patency variability, and bronchial hyper-reactivity [23, 24]. Due to the fact that respiratory inflammation plays a key role in asthma pathogenesis, inflammation monitoring is to be the main component of patients' management. Currently, the most extensively studied inflammation biomarker in BA is the level of nitric oxide and its metabolites in exhaled air [25–28]. Therefore, cellular composition of induced sputum, the components of expiratory air condensate (pH, leukotrienes, aldehydes and other parameters) are being under study [29–35]. A new analytical method to detect biomarkers in expiratory air condensate is metabolomics [36]. Biomarkers can be also used to diagnose basic phenotypes and endotypes of asthma. For example, the levels of Feno, serum periostin, eosinophilic neurotoxin and osteopontin can be used to diagnose and monitor Th2-dependent eosinophilic inflammation in BA [37, 38].
Allergic inflammation persistence in the respiratory tract underlies the uncontrolled BA course. To obtain complete control over asthma is the primary objective of asthma treatment [23]. Considering that respiratory inflammation is the main pathogenic component determining BA course there is the necessity for anti-inflammatory treatment as baseline therapy [39]. To obtain and maintain the control over BA symptoms and course the following pharmaceuticals are used: inhaled glucocorticosteroids (GCS), leukotriene receptor antagonists, cromones, beta-2-agonists and long-acting theophyllines [40, 41]. In severe asthma and resistant to the mentioned pharmaceuticals, systemic GCS and anti-IgE-therapy are used [42]. Moreover, for pathogenetic BA therapy other drugs are being developed now — pharmaceutical drugs with anti-cytokine and anti-mediator effects [43].
Glucocorticosteroids
Glucocorticosteroids exhibit high anti-inflammatory and anti-allergic action related to its capacity to activate anti-inflammatory genes and suppress many pro-inflammatory genes initiated in the course of inflammation (Table 1). As a result, there is the inhibition of synthesis of pro-inflammatory cytokines and lipid mediators (leukotriene, prostaglandins), retardation of eosinophil participation in the development of allergic inflammation and excretion of eosinophilic mediators [44–46].
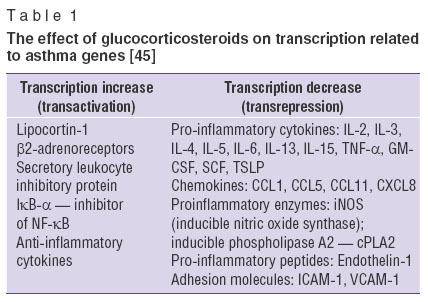 Table 1. The effect of glucocorticosteroids on transcription related to asthma genes [45] Table 1. The effect of glucocorticosteroids on transcription related to asthma genes [45]
|
Primarily, in BA inhaled GCS are administered to neutralize systemic side effects common to GCS. As a result of treatment, on day 5–7 of therapy most patients with incomplete BA control were found to have broncho-obstructive syndrome disappeared. By the third week of treatment there was respiratory function normalization, and nonspecific bronchial hyper-reactivity decrease. The therapy of starter doses of inhaled GCS generally lasts for 3 months, and in case there are no symptoms, the daily dose is reduced to a maintaining dose to prevent asthma recurrence. Patients can receive a maintaining dose for a few years. The application of inhaled GCS improves the quality of life in BA patients.
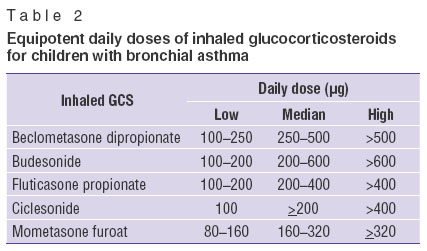
Currently, the following inhaled GCS are used to provide anti-inflammatory baseline therapy in BA children: beclometasone dipropionate, budesonide, ciclesonide, fluticasone propionate, mometasone furoate. These medications have high affinity for GCS receptors, and are able to reach high and long keeping therapeutic concentrations in tissues when locally administered. They rapidly inactivate due to biotransformation in the liver after systemic absorption. High local anti-inflammatory activity and low systemic bioavailability are the main factors of efficacy and safety of inhaled GCS [45]. Table 2 shows equipotent daily doses of these drugs for children with BA.
|
|
Beclometasone dipropionate is inhaled GCS with high anti-inflammatory activity and an insignificant systemic effect. It has been used in BA therapy for 40 years and shown its clinical efficiency and safe profile in children and adults with chronic persistent asthma [47, 48]. Beclometasone dipropionate is a prodrug, which hydrolyzes in the lungs to beclometasone monopropionate. And beclometasone monopropionate, in its turn, hydrolyzes to beclometasone. A daily dose of beclometasone dipropionate is 200–1200 μg and administered 3–4 intakes.
Beclometasone dipropionate is an active substance in aerosol spray Clenil Get. A jet-system increases aerosol deposition in the lungs and reduces deposition of its particles in oropharynx that enables to reduce the risk of oropharyngeal candidosis, cough, hoarseness, and systemic effect of the drug. One inhalation dose contains 200 or 250 μg beclometasone dipropionate. 6–12-year-old-children are administered 250 μg b.i.d., a daily dose for children over 12 years with mild form of the disease is 200–600 μg for 2 inhalations, in moderate asthma — 600–1000 μg for 2–4 inhalations, in severe asthma — 1000–2000 μg for 2–4 inhalations [49].
Clenic UDV based on beclometasone dipropionate for nebulizer BA therapy is produced in the form of suspension in ampoules containing 800 μg of beclometasone dipropionate. Children over 6 years are administered the medication by a half of an ampoule for nebulation at the dose of 400 μg 1–2 times a day [48].
Budesonide is the only non-halogenated inhaled GCS, has been used in asthma therapy for 35 years. 90% of budesonide metabolizes in the liver and excretes from the body in the form of inactive metabolites. When interacting with fatty acids in cells, budesonide forms complexes, which are intracellular drug reservoir [50].
Pulmicort Turbuhaler is budesonide powder delivered in bronchi by turbuhaler. One inhalation dose of Pulmicort Turbuhaler contains about 200 μg of the agent. Pulmicort Turbuhaler is administered to children over 7 years at the dose of 400–800 μg for 2–4 intakes.
Pulmicort-based suspension manufactured in nebulas (for nebulizer therapy) has become widely used to treat BA exacerbations in children. There has also been used an analogue of Pulmicort — Budenit Steri-Neb, dosing suspension. To treat BA in children Pulmicort suspension dose is selected individually: an initial dose for 6-month-children and older is 0.25–0.5 mg/day. If necessary, a dose can be increased to 1 mg/day.
Benacort is a budesonide-based domestic GCS drug. It is powder in a cyclohaler containing 400 budesonide doses. Sodium benzoate is used as a filler, as it has antifungal activity [51]. Another form of Benacort is inhalation powder in the form of capsules (200 doses) used for children over 7 years, a daily dose being 400–800 μg for 2–3 intakes [52].
Fluticasone propionate exhibits marked anti-inflammatory activity [53]. The administration of this inhaled GCS for 6 months and more enables to obtain BA control and reach clinical remission.
Fluxotide is dosing aerosol manufactured in bottles containing 60 (120) inhalation doses of 125/250 μg of the agent. It comes pre-loaded with blisters containing individual doses of the medicine as a powder. One dose may contain 50, 100, 250 and 500 μg of fluticasone propionate. Depending on BA severity, Flixotide is administered in children over 4 years, a daily dose being 100–500 μg for 2 intakes.
Ciclesonide is an extra-finely divided inhaled GCS. Ciclesonide deposits both in central and peripheral bronchial parts. It is a prodrug by its mechanism of action, as it activates in endothelial cells of the respiratory tract forming an active metabolite — des-ciclesonide with hundredfold affinity to GCS receptors compared to ciclesonide. Ciclesonide therapy promotes BA control, it having high clinical efficiency.
Alvesco is manufactured in aerosol packs containing 40, 80 and 160 μg in one inhalation dose. It is used in BA in 6-year-old children and over. A dose is 80–300 μg depending on BA severity [54, 55].
Mometasone furoate is GCS with the highest affinity for GCS receptors compared to other inhaled GCS used in BA. Its long half lifetime correlates with high therapeutic efficiency and safety.
The advantage of Asmanex Twisthaler is the possibility to use it once a day that contributes to patients’ compliance increase. Pharmaceutical form (200 and 400 μg) complies with the requirements for sequential BA therapy, and enables to increase or reduce a dose due to the characteristics of asthma control [56].
Therapy of low and median doses of inhaled GCS minimizes systemic side effects. However, when administering inhaled GCS therapy one should take into consideration a child's height and recommend to use minimum effective doses in all children with BA [57]. Inhaled GCS are the most effective anti-inflammatory drugs providing control over the symptoms and courses of most BA cases. However, there are cases of steroid-resistance requiring dose increase that is presents an increase in risk of unfavorable side effects.
Understanding of molecular mechanisms of GCS action enables to consider in detail the causes of GCS resistance formation [58]. Currently, there has been found that innate steroid-resistance related to mutation in the gene encoding GCS receptors is very rare in BA [59, 60]. More frequently, there is acquired steroid-resistance, which is, primarily, due to GCS receptor modification in asthma: when exposed to Th2-proinflammatory cytokines, the products of nitrosylating and oxidative stress, microbial and fungal super-antigens, and their degradation in response to proteases [61]. The problem of steroid-resistance now is being attempted to solve in two ways. On the one hand, BA phenotypes and endotypes are being studied intensively in order to determine the cohorts of patients, whose pathogenetic characteristics of the disease are responsible for initial resistance to GCS (e.g., Th17-mediated, primarily, neutrophil variants of inflammation in BA) [62]. On the other hand, there have been intensively developed new approaches to increase anti-inflammatory GCS activity, decrease the probability of unfavorable side effects of these drugs. The work is being carried out in three directions.
1. Combination therapy: the second medicinal product is added to inhaled GCS to overcome steroid-resistance and reduce GCS doses necessary to reach the clinical effect. Long acting beta-2-agonists exhibit such properties. Currently, novel pharmaceuticals are under clinical trials, such as selective inhibitors p38-МАРК (mitogen-activated protein kinase) [63]. Inhibitor p38-МАРК has an effect on transcription of genes encoding synthesis of many pro-inflammatory cytokines including TNF-α, IL-4, IL-5, IL-8, RANTES and eotaxin, and so asthma pathogenesis as well. Some manifestations of steroid-resistance can be neutralized by small doses of theophylline [64]. Application of antioxidants is considered as emerging [61].
2. Development of prodrugs (by ciclesonide type, which turns into its active form in the lungs — С21-de-methylpropionyl-ciclesonide accompanied by low oral-pharyngeal absorption), as well as medications with high affinity to GCS receptors that enables to administer the drugs once a day (ciclesonide, fluticasone furoate, mometasone furoate) [65].
3. Development of dissociated GCS, which would have effects different in their intensity on gene transrepression and transactivation that would enable to modulate unfavorable side effects of these drugs as well [45].
Fixed dose combination of GCS and long-acting beta-2-agonists
Combination therapy is one of the approaches to improve the efficiency of inhaled GCS and surmount their steroid-resistance in BA. The most applicable in practice are fixed combinations of GCS and long-acting beta-2-agonists: fluticasone propionate and salmeterol xinafoat (Seretide, Tevacomb), budesonide and formoterol fumarate (Symbicort), beclometasone dipropionate and formoterol fumarate (Foster). Combined therapy by combination drugs is the most effective treatment of children with severe and moderate severe BA compared to isolated application of inhaled GCS.
Fluticasone propionate + salmeterol xinafoat (original combination: Seretide, GlaxoSmithKline, Great Britain) is manufactured as dry powder inhalator — Seretide Multidisk, one dose containing 50 μg of salmeterol xinafoat and 100, 250 and 500 μg of fluticasone pronionate, and as dose aerosol inhaler (without freon), each dose containing 25 μg of salmeterol xinafoat and 50, 125 and 250 μg of fluticasone pronionate. It is used tostable doses since the age of four. Seretide dose is determined due to child's age and BA severity. Therapy success appears as reduced number of BA symptoms and exacerbations, and the achievement of clinical remission in some patients. It has high tolerability.
Formoterol fumarate + budesonide (original combination: Symbicort Turbuhaler, Astra Zeneca, Sweden) is used for inhalations in children since the age of 6. 6–12-year-old children are administered the medicinal product according to the following schedule: 80/4.5 μg/dose by 1–2 inhalations twice a day, children of 12 years and over — 160/4.5 μg/dose by 1–2 inhalations twice a day. Symbicort Turbuhaler therapy can be administered in flex dosing, with a dosage being increased during the disease recurrence (up to 2 inhalations twice a day) and reduced to a maintaining dose (by 1 inhalation once a day) in stable patients. It has high tolerability.
Beclometasone dipropionate + formoterol fumarate (original combination: Foster, Сhiesi, Italy) is a fixed dose combination of extra-finely-divided beclometasone dipropionate, 100 μg, and formoterol fumarate, 6 μg, as a single dose in an aerosol inhaler (Modulit technology). It is used in children over 12 years, by 1–2 inhalations twice a day. Therapy contributes to decreased BA symptom prevalence rate, and reduced number of BA exacerbations; the combination showing high tolerability [66–68].
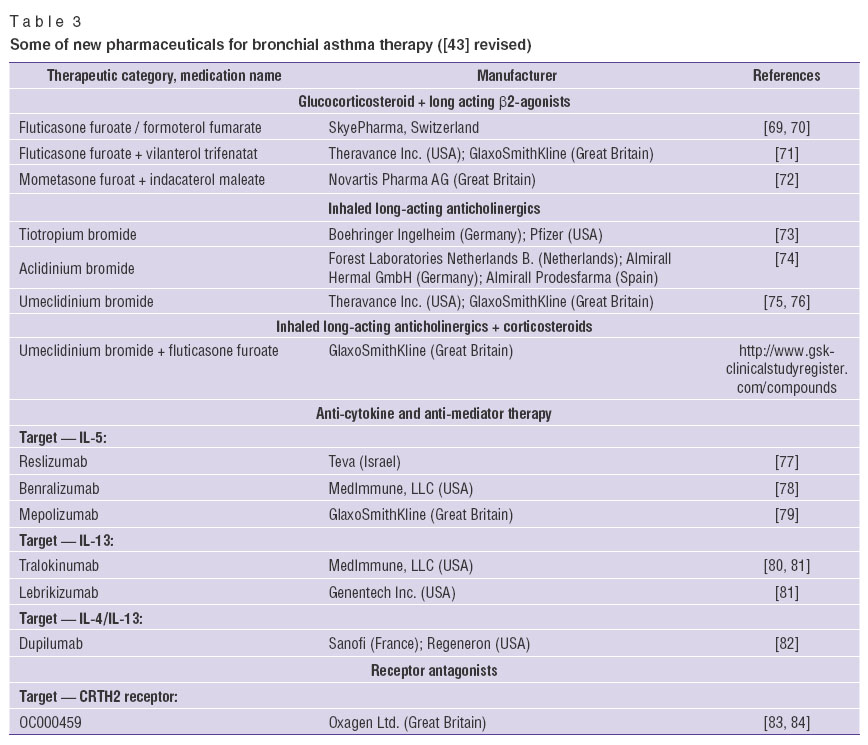
Over the last years, new fixed combinations have appeared in pharmaceutical market (Table 3).
|
|
Fluticasone furoate + vilanterol trifenatate is the combination of inhaled GCS and ultra-long-acting beta-2-agonist (original combination: Breo Ellipta, GlaxoSmithKline, Great Britain) administered once a day. There have been carried out clinical trials, phase III, in adolescents aged 12 and older, as well as in adult patients with asthma. The efficacy of a single administration of 100/25 μg a day is comparable to that of 250/50 μg of fluticasone propionate + salmeterol twice a day in patients with persistent asthma uncontrolled by medium doses of inhaled GCS after 24-week therapy [71].
Mometasone furoate + formoterol fumarate is an original combination of Zenhale, 3M Health Care Ltd. (USA); Organon (Ireland). The recommended dosages of 100/5 and 200/5 μg twice a day to treat BA in adolescents and adults [72].
Fluticasone propionate + formoterol fumarate is an original combination, Flutiform, SkyePharma (Switzerland). The dose of 250/10 μg has been shown to provide higher efficiency than monotherapy (fluticasone propionate) to control moderate severe and severe BA, with safety profile similar to fluticasone propionate monotherapy [69, 70].
The administration of inhaled GCS and fixed-dose combination is reasonable, primarily, in persistent moderate severe or severe BA. They are ineffective in mild persistent asthma, though not so much needed, since the control can be obtained by non-steroid anti-inflammatory therapy as well (cromones, leukotriene receptor antagonists).
The alternative of long-acting beta-2-agonists in some cases is supposed to be long-acting anticholinergics including those combined with inhaled GCS. Currently, the idea provokes considerable interest [85–87]. Accordingly, long-acting anticholinergics are being actively studied.
Tiotropium bromide, including that combined with inhaled GCS, is under phase III of clinical trials to study its possible application in asthma therapy in children and adolescents. When administered in adult subjects, it resulted in significant decrease of exacerbation rate [73].
Umeclidinium bromide is currently being under clinical trials, phase II, for possible use in asthma treatment as both monotherapy and a part of combination therapy with inhaled GCS [75, 76].
Aclidinium bromide. The researches carried out have demonstrated its bronchodilating and anti-inflammatory effect [74].
Non-steroidal anti-inflammatory drugs
Leukotriene receptor antagonists have widespread application in bronchial asthma therapy in children.
Montelukast sodium (Singulair, Montelar, Montelast, Singlon) inhibits cysteinyl leukotriene receptors used in children since 2 years. Its dose for 2–5-year-old children is 4 mg in a chewable tablet, at the age of 6–14 years — 5 mg in a chewable tablet, once a day, for children of 15 years and over — one coated tablet, 10 mg daily. The medication prevents day and night BA symptoms, reduces exacerbations in aspirin-sensitive, virus-induced asthma and exercise induced asthma, minimizes manifestations of associated allergic rhinitis, persistent and intermittent rhinitis [88, 89]. Montelukast sodium is used as monotherapy to control mild asthma; in combination with inhaled GCS can be effective in moderate severe or severe BA enabling to reduce GCS dose. This medication is used also in case of GCS withdrawal or dose reduced to maintain BA control attained. Montelukast sodium exhibits high tolerability, headache and nausea occurring rarely [90].
Theophylline has been used to treat respiratory diseases for over 100 years. It was initially administered as bronchodilator. However, relatively high doses necessary for bronchial obstruction arrest cause unfavorable side effects; therefore its application for that purpose has been reduced. However, theophylline in lower concentrations is characterized by anti-inflammatory effects due to PDE4 inhibition and histone deacetylase-2 activation, with the result that activated inflammatory genes are knocked out. Through this mechanism theophylline reduces steroid-resistance that can be of particular concern in patients with severe asthma. Methylxanthine medications inhibit А1-receptors to adenosine causing a bronchodilating effect, suppress the release of inflammatory mediators by mast cells and basophils, and enhance apoptosis of eosinophils inhibiting respiratory inflammation. Currently, in BA therapy there used primarily low doses of slowly released theophylines (Neotheo-Pecum А, Theopec, Ventax, Teotard, Etiphylline, etc.). In children with BA prolonged theiphyllines can be administered for the anti-inflammatory purpose at low doses as a component of baseline therapy for 1–2 months. Repository theophylline therapy contributes to reduced number of asthmatic attacks, the increase of effort tolerance, and in some patients inhaled GCS dose reduction. Theophylline tolerance in such doses in most children is high. In individual cases there can be sleep disturbance, tachycardia, nausea, vomiting, headaches due to phosphodiesterase inhibition, higher doses can cause cardiac arrhythmia [64].
Additional administration of Montelukast sodium and repository theophylline enables to improve therapy efficacy and obtain asthma control in children with severe BA with inadequate efficacy of inhaled GCS and long-acting beta-2-agonists.
Roflumilast, phosphodiesterase 4 inhibitor, has approved indication for patients with chronic obstructive pulmonary disease. Its potential anti-inflammatory effects have been shown in a randomized placebo-controlled clinical study in patients with mild allergic asthma [91].
Cromones (cromoglicic acid and sodium nedocromil) are able in exposition with causally significant allergen to prevent bronchospasm development, an early and late phase of allergic reaction, inhibit the increase of bronchoreactivity. They are effective primarily in children with mild BA [92]. These medications have an insignificant effect on disease exacerbation once developed [93].
Cromoglicate sodium is manufactured both as dose aerosol, and 2% solution of nebulized 2 ml-inhalations. Inhalation frequency of cromoglicic acid is 4 times a day. Baseline therapy requires long administration, at least 3 months. In mild asthma, cromoglicate sodium is used to prevent seasonal exacerbations of the disease and BA exacerbations on physical exertion. The medication has high tolerability. Side effects are rare, and occur mainly as local reaction in the form of reactive airway disease, cough, and rarely — a bronchospasm [94].
Nedocromil sodium (Tilade) suppresses the release of inflammation mediators from mast cells, eosinophils, neutrophils, monocytes, macrophages and platelets, inhibits bronchospasm development, late allergic reactions, and reduces nonspecific hyper-reactivity of bronchi and BA exacerbation rate. The medication is manufactured as dosed aerosol, 2 ml, for children over 2 years (1 inhalation dose) 2–4 times a day [93].
Biological treatment modalities in bronchial asthma
Anti-IgE-therapy. In severe, refractory to conventional pharmacotherapy BA course, anti-IgE-therapy based on parenteral administration of anti-IgE-antibodies in the form of omalizumab (Xolair) can be effective. Omalizumab binds free-circulating IgE in blood, reduces the production of high-affinity receptors on membrane of mast cells and basophils resulting in decreased excretion of mediators, allergic inflammation intensity and BA exacerbation regression [95–97]. Before treatment initiation, an individual dose of omalizumab is calculated considering total IgE level in peripheral blood and child's body mass, the medication being administered subcutaneously. Omalizumab promotes the reduction of BA exacerbation rate, the number of admissions to hospital and visits to a doctor, decrease of baseline therapy when obtaining complete control over the disease in most cases. In some cases after the medication administration patients may suffer from headache, and in the site of its subcutaneous injection there may occur edema, erythema and itching. The main indication for omalizumab administration is severe BA in children aged 6 and over, refractory BA to pharmacotherapy [98].
Anti-cytokine therapy. Based on common knowledge on Th2-dependent asthma genesis and eosinophillic respiratory inflammation in this disease, anti-cytokine therapy, in addition to IgE, also targets interleukins IL-5, IL-13, IL-4, IL-9 [99].
Anti-interleukin-5-antibodies. IL-5 is involved in the activation and maturation of eosinophils. Anti-IL-5-antibodies — Mepolizumab is being under clinical study, phase III, DREAM, which involved patients aged 12–74 years with recurrent severe BA and the signs of eosinophilic inflammation. It showed the therapy efficacy including BA exacerbation reduction by 52% annually [79, 100]. Currently, within the frame of III phase of clinical trials there being studied the antibodies to IL-5 receptor (Benralizumab); within a few months after a single injection of the medication there are the effects of eosinophil exhaustion [78].
Anti-interleukin-13-antibodies. IL-13, an essential BA mediator, produces the most of BA characteristics in experimental models including mucus remodeling, hyperproduction, IgE synthesis, recruitment of eosinophils and basophils [101]. For effective assessment of anti-IL-13-therapy, periostin, a novel serum asthma biomarker is used, which is a component of extracellular matrix isolated from epithelial respiratory cells in response to IL-13 and IL-4, its release is inhibited by GCS [102, 103]. Serum periostin content enables to differentiate patients with “expressed” and “unexpressed” Th2-phenotype of BA [12, 104]. Specific anti-IL-13-antibodies are the following drugs: Lebrikizumab, Tralokinumab, Anrukinzumab [80, 81]. Lebrikizumabis injected subcutaneously once a month. A randomized multi-center study (219 patients) has shown it to be more effective in patients with higher initial periostin level in blood serum [100, 80, 105].
Anti-interleukin-4-antibodies. IL-4 is involved in differentiation of Th2-cells switching to IgE synthesis, recruitment of eosinophils and mast cells. Altrakincept is soluble recombinant human receptor to IL-4 meant for inhalation therapy. The medication neutralizes the activation of immune and other cells caused by IL-4. A single inhalation in adults with moderate asthma results in pulmonary function improvement and reduced level of expired nitric oxide [106]. Pitrakinra — an antagonist of heterodimeric receptor complex (IL-4R-IL-13Ра) — has been developed to overcome biological redundancy of IL-4 and IL-13 that is likely to compensate inefficiency of strategies targeting IL-4 [107]. Pitrakinra inhibits allergen-induced allergic reactions and disease exacerbations in adults with eosinophilic asthma [108]. AMG 317 is a monoclonal antibody targeting receptors to IL-4; it blocks IL-4 binding with its receptor, as well as inhibits IL-13 signal transduction. In adult patients with moderate and severe asthma, AMG 317 produces significant clinical improvement only in a group of patients without disease control [109]. Dupilumab is one of the last medications of anti-IL-4-therapy; it has an effect on alpha-subunit of IL-4 receptor. Its administration in patients with eosinophilic asthma due to inhibition of both IL-4 and IL-13 is accompanied by significant reduction of BA exacerbations and improved pulmonary function in adults with persistent asthma, withdrawal of beta-agonists and reduced dose of inhaled GCS [82].
OC000459 is an oral CRTH2 (chemo-attractant receptor of Тh2-helper homologous molecule) antagonist. In a randomized double blind clinical trial (phase II) in adults with moderate persistent asthma, the use of oral antagonist of CRTH2 was accompanied by improved pulmonary function, the alleviation of night symptoms and the improvement of life quality compared to placebo [83, 84].
MEDI-528 is anti-IL-9-antibodies. The use of this medication has shown the tendency for improvement of control indices in adult patients with mild and moderate asthma, as well as a protective effect against bronchospasm [110].
Potential targets of new approaches to BA therapy under development are TSLP, IL-25 and IL-33 molecules produced by epithelial respiratory cells in response to allergens or viral triggers, therefore they can be considered as possible targets when developing novel asthma treatment modalities [103, 111].
Targeted neutrophilic inflammation therapy. Neutrophilic inflammation in BA is associated with interleukins IL-17 and IL-23. Secukinumab — anti-IL-17-antibodies — are being currently under clinical trial, phase II [112].
It should be noted that national and international conciliation documents recommend a staged approach to achieve and maintain BA control. Transition to the next or previous stage can be made within a given period depending on BA severity, against the assessment of the disease control under routine medical supervision. Control achievement in atopic asthma is promoted by allergen-specific immune therapy by causally significant allergens and their level reduction in the patient's environment [15, 99, 113–115]. BA monitoring in children includes pulmonary function test, exhaled nitric oxide concentration test, and bronchoreactivity assessment [27, 116]. Obtaining and maintenance of asthma control are promoted by educational programs for parents and asthmatic children. In case of BA attacks, there being applied the inhalation therapy of short-acting beta-2-agonists or fixed dose combinations (Berodual) using dosed inhalers and nebulizers. In severe asthmatic attacks, inhaled and systemic GCS (per оs or parenterally) therapy is administered. In status asthmaticus, infusion therapy by Euphylline and GCS appears to be effective.
Conclusion. Despite a wide range of medications for anti-inflammatory baseline therapy and emergency drugs, it is still a problem of uncontrolled and poorly controlled bronchial asthma course, so it determines the necessity for developing additional diagnostic and therapeutic approaches. In this regard, to optimize pathogenetic therapy of bronchial asthma, the work is being currently carried out to improve the existing anti-inflammatory drugs and their combinations. Moreover, there is a search for crucially new approaches to asthma treatment with due consideration of the disease phenotypes and endotypes including development and practical application of pharmaceutical drugs with anti-cytokine and anti-mediator effects. It is hoped that as far as the knowledge of molecular characteristics of asthma endotypes is being refined, and there being introduced the biomarkers enabling to diagnose asthma phenotypes and endotypes and monitor asthma control, there will be implemented an individual approach in individual therapy administration.
References
- Asher M.I. The asthma epidemic — global and time trends of asthma in children. In: Global atlas of asthma. Akdis C.A., Agache I. (editors). EAACI; 2013; p. 7–9.
- Lambrecht B.N., Hammad H. The immunology of asthma. Nat Immunol 2014; 16(1): 45–56, http://dx.doi.org/10.1038/ni.3049.
- Gushchin I.S. Allergic permeability of barrier tissues is strategic problem of allergology. Pul’monologiya 2006; 3: 5–13.
- Holgate S.T. Innate and adaptive immune responses in asthma. Nat Med 2012; 18(5): 673–683, http://dx.doi.org/10.1038/nm.2731.
- Esposito S., Tenconi R., Lelii M., Preti V., Nazzari E., Consolo S., Patria M.F. Possible molecular mechanisms linking air pollution and asthma in children. BMC Pulm Med 2014; 14(1): 31, http://dx.doi.org/10.1186/1471-2466-14-31.
- Wenzel S.E. Asthma phenotypes: the evolution from clinical to molecular approaches. Nat Med 2012; 18(5): 716–725, http://dx.doi.org/10.1038/nm.2678.
- Anderson G.P. Endotyping asthma: new insights into key pathogenic mechanisms in a complex, heterogeneous disease. Lancet 2008; 372(9643): 1107–1119, http://dx.doi.org/10.1016/s0140-6736(08)61452-x.
- Leung T.F., Ko F.W.S., Wong G.W.K. Recent advances in asthma biomarker research. Ther Adv Respir Dis 2013; 7(5): 297–308, http://dx.doi.org/10.1177/1753465813496863.
- Li B.W.S., Hendriks R.W. Group 2 innate lymphoid cells in lung inflammation. Immunology 2013; 140(3): 281–287, http://dx.doi.org/10.1111/imm.12153.
- Vroman H., van den Blink B., Kool M. Mode of dendritic cell activation: the decisive hand in Th2/Th17 cell differentiation. Implications in asthma severity? Immunobiology 2015; 220(2): 254–261, http://dx.doi.org/10.1016/j.imbio.2014.09.016.
- Essilfie A.-T., Simpson J.L., Horvat J.C., Preston J.A., Dunkley M.L., Foster P.S., Gibson P.G., Hansbro P.M. Haemophilus influenzae infection drives IL-17-mediated neutrophilic allergic airways disease. PLoS Pathog 2011; 7(10): e1002244, http://dx.doi.org/10.1371/journal.ppat.1002244.
- Woodruff P.G., Modrek B., Choy D.F., Jia G., Abbas A.R., Ellwanger A., Koth L.L., Arron J.R., Fahy J.V. T-helper type 2-driven inflammation defines major subphenotypes of asthma. Am J Respir Crit Care Med 2009; 180(5): 388–395, http://dx.doi.org/10.1164/rccm.200903-0392oc.
- Mantzouranis E., Papadopouli E., Michailidi E. Childhood asthma: recent developments and update. Curr Opin Pulm Med 2014; 20(1): 8–16, http://dx.doi.org/10.1097/mcp.0000000000000014.
- Balabolkin I.I. Bronkhial’naya astma u detey [Asthma in children]. Moscow; 2003; 320 p.
- Gushchin I.S., Kurbacheva O.M. Allergiya i allergenspetsificheskaya immunoterapiya [Allergy and allergen-specific immune therapy]. Moscow; 2010; 228 p.
- Kuipers H., Lambrecht B.N. The interplay of dendritic cells, Th2 cells and regulatory T cells in asthma. Curr Opin Immunol 2004; 16(6): 702–708, http://dx.doi.org/10.1016/j.coi.2004.09.010.
- Kudo M., Ishigatsubo Y., Aoki I. Pathology of asthma. Front Microbiol 2013; 4: 263, http://dx.doi.org/10.3389/fmicb.2013.00263.
- Rowe R.K., Gill M.A. Asthma: the interplay between viral infections and allergic diseases. Immunol Allergy Clin North Am 2015; 35(1): 115–127, http://dx.doi.org/10.1016/j.iac.2014.09.012.
- Aydogan M., Ozen A., Akkoc T., Eifan A.O., Aktas E., Deniz G., Gocmen I., Bahceciler N.N., Barlan I. Risk factors for persistence of asthma in children: 10-year follow-up. J Asthma 2013; 50(9): 938–944, http://dx.doi.org/10.3109/02770903.2013.831872.
- Eliseeva T.I., Balabolkin I.I., Prakhov A.V. Struktura sensibilizatsii k aeroallergenam u detey s bronkhial’noy astmoy. V kn.: Aktual’nye voprosy pediatrii, perinatologii i reprudoktologii: mezhvuzovskiy sbornik nauchnykh trudov [Structure of sensibilization to aeroallergens in children with bronchial asthma. In: Topical issues of pediatrics, perinatology and reproductology: interuniversity collection of scientific papers]. Nizhny Novgorod; 2013; p. 31–38.
- Eliseeva T.I., Bol’shova E.V., Kul’gina Yu.S., Konyshkina T.M., Prakhov A.V., Novikova N.A. Antibodies to Chlamydophila pneumoniae and Mycoplasma pneumoniae in children with different control level of bronchial asthma. Meditsinskiy al’manakh 2011; 4(17): 235–238.
- Bulgakova V.A. Clinical value of study of immunocompetent cell apoptosis activation markers in atopical bronchial asthma in children. Pediatriya 2009; 87(2): 12–18.
- GINA. Global strategy for asthma management and prevention 2014 (Revision 2014), http://www.ginasthma.org/local/uploads/files/GINA_Report_2014_Aug12.pdf.
- Eliseeva T.I., Balabolkin I.I., Prakhov A.V. Variabel’nost’ bronkhial’noy prokhodimosti pri otsenke urovnya kontrolya bronkhial’noy astmy u detey. V kn.: Prakticheskie zadachi i aktual’nye voprosy detskoy allergologii i immunologii [Bronchial patency variability in bronchial asthma control assessment in children. In: Practical problems and topical issues of pediatric allergology and immunology]. Moscow; 2013; p. 19.
- Ritz T., Trueba A.F. Airway nitric oxide and psychological processes in asthma and health: a review. Ann Allergy Asthma Immunol 2014; 112(4): 302–308, http://dx.doi.org/10.1016/j.anai.2013.11.022.
- Turner S. Exhaled nitric oxide in the diagnosis and management of asthma. Curr Opin Allergy Clin Immunol 2008; 8(1): 70–76, http://dx.doi.org/10.1097/aci.0b013e3282f3b4b0.
- Eliseeva T.I., Geppe N.A., Soodaeva S.K. Integrated assessment of control over bronchial asthma in children based on the determination of nitric oxide metabolite content in exhaled breath condensate and spirographic parameters. Pul’monologiya 2013; 6: 51–56.
- Volkova L.I., Kapitanova D.V., Boyarko V.V., Saprykina E.V. Cellular composition of induced sputum and nitric oxide in exhaled breath condensate in bronchial asthma. Sibirskiy meditsinskiy zhurnal 2007; 4: 17–21.
- Rahman I., Kelly F. Review Biomarkers in breath condensate: a promising new non-invasive technique in free radical research. Free Radic Res 2003; 37(12): 1253–1266, http://dx.doi.org/10.1080/10715760310001623331.
- Corradi M., Zinelli C., Caffarelli C. Exhaled breath biomarkers in asthmatic children. Inflamm Allergy Drug Targets 2007; 6(3): 150–159, http://dx.doi.org/10.2174/187152807781696437.
- Grob N.M., Aytekin M., Dweik R. Biomarkers in exhaled breath condensate: a review of collection, processing and analysis. J Breath Res 2008; 2(3): 1–18, http://dx.doi.org/10.1088/1752-7155/2/3/037004.
- Anaev E.Kh. The study of exhaled breath condensate РН in pulmonary inflammatory diseases. Pul’monologiya 2005; 5: 75–79.
- Eliseeva T.I. A new technique for determining Н2О2 in exhaled breath condensate. Allergologiya i immunologiya v pediatrii 2008; 14(3): 44.
- Eliseeva T.I. Diagnostic objectivization of bronchial asthma control level in children using рН-metry of exhaled breath condensate. Sovremennye meditsinskie tekhnologii 2010; 3: 44–47.
- Murugan A., Prys-Picard C., Calhoun W.J. Biomarkers in asthma. Curr Opin Pulm Med 2009; 15(1): 12–18, http://dx.doi.org/10.1097/mcp.0b013e32831de235.
- Luxon B.A. Metabolomics in asthma. Adv Exp Med Biol 2014; 795: 207–220, http://dx.doi.org/10.1007/978-1-4614-8603-9_13.
- Kim M.A., Shin Y.S., Pham le D., Park H.S. Adult asthma biomarkers. Curr Opin Allergy Clin Immunol 2014; 14(1): 49–54, http://dx.doi.org/10.1097/ACI.0000000000000028.
- Lang J.E., Blake K.V. Role of biomarkers in understanding and treating children with asthma: towards personalized care. Pharmgenomics Pers Med 2013; 6: 73–84, http://dx.doi.org/10.2147/pgpm.s30626.
- Balabolkin I.I., Bulgakova V.A., Tyumentseva E.S. Bronchial asthma therapy in children: modern approaches to treatment. Meditsinskiy sovet 2010; 1–2: 34–39.
- Crompton G. A brief history of inhaled asthma therapy over the last fifty years. Prim Care Respir J 2006; 15(6): 326–331, http://dx.doi.org/10.1016/j.pcrj.2006.09.002.
- Kupczyk M., Dahlén B., Dahlén S.E. Which anti-inflammatory drug should we use in asthma? Pol Arch Med Wewn 2011; 121(12): 455–459.
- Olin J.T., Wechsler M.E. Asthma: pathogenesis and novel drugs for treatment. BMJ 2014; 349: g5517, http://dx.doi.org/10.1136/bmj.g5517.
- Wechsler M.E. Getting control of uncontrolled asthma. Am J Med 2014; 127(11): 1049–1059, http://dx.doi.org/10.1016/j.amjmed.2014.05.006.
- Shahid S.K. Newer glucocorticosteroids and corticosteroid resistance reversal in asthma. Pharm Pat Anal 2013; 2(3): 373–385, http://dx.doi.org/10.4155/ppa.13.14.
- Barnes P.J. Glucocorticosteroids: current and future directions. Br J Pharmacol 2011; 163(1): 29–43, http://dx.doi.org/10.1111/j.1476-5381.2010.01199.x.
- Emel’yanov A.V. Efficacy and safety of inhaled glucocorticosteroids. Rossiyskiy allergologicheskiy zhurnal 2005; 2: 3–21.
- Brown H.M., Storey G., George W.H.S. Beclomethasone dipropionate: a new steroid aerosol for the treatment of allergic asthma. Br Med J 1972; 1: 585–590, http://dx.doi.org/10.1136/bmj.1.5800.585.
- Nicolini G., Cremonesi G., Melani A.S. Inhaled corticosteroid therapy with nebulized beclometasone dipropionate. Pulm Pharmacol Ther 2010; 23(3): 145–155, http://dx.doi.org/10.1016/j.pupt.2009.11.003.
- Vaghi A., Berg E., Liljedahl S., Svensson J.O. In vitro comparison of nebulised budesonide (Pulmicort Respules) and beclomethasone dipropionate (Clenil per Aerosol). Pulm Pharmacol Ther 2005; 18(2): 151–153, http://dx.doi.org/10.1016/j.pupt.2004.10.004.
- Ellul-Micallef R., Hansson E., Johansson S.A. Budesonide: a new corticosteroid in bronchial asthma. Eur J Respir Dis 1980; 61(3): 167–173.
- Kislyak L.V., Sokolov A.S., Chuchalin A.G. Benacort in out-patient treatment of patients with bronchial asthma. Pul’monologiya 2002; 1: 90–94.
- Svetlakov V.I. Benacort™ is the first Russian inhaled nebulized glucocorticosteroid. Pul’monologiya 2005; 2: 113–116.
- Fabbri L.M., Burge P.S., Croonenborgh L., Warlies F., Weeke B., Ciaccia A., Parker C. Comparison of fluticasone propionate with beclomethasone dipropionate in moderate to severe asthma treated for one year. International Study Group. Thorax 1993; 48(8): 817–823, http://dx.doi.org/10.1136/thx.48.8.817.
- Buczyłko K. Safety and efficacy of inhaled ciclesonide in asthma. Pol Merkur Lekarski 2003; 14(84): 623–626.
- Gelfand E.W., Georgitis J.W., Noonan M., Ruff M.E. Once-daily ciclesonide in children: efficacy and safety in asthma. J Pediatr 2006; 148(3): 377–383, http://dx.doi.org/10.1016/j.jpeds.2005.10.028.
- Milgrom H. Mometasone furoate in children with mild to moderate persistent asthma: a review of the evidence. Paediatr Drugs 2010; 12(4): 213–221, http://dx.doi.org/10.2165/11316220-000000000-00000.
- Pruteanu A.I., Chauhan B.F., Zhang L., Prietsch S.O., Ducharme F.M. Inhaled corticosteroids in children with persistent asthma: dose-response effects on growth. Evid-Based Child Health 2014; 9(4): 931–1046, http://dx.doi.org/10.1002/ebch.1989.
- Barnes P.J., Adcock I.M. Glucocorticoid resistance in inflammatory diseases. Lancet 2009; 373(9678): 1905–1917, http://dx.doi.org/10.1016/s0140-6736(09)60326-3.
- Lamberts S.W. Hereditary glucocorticoid resistance. Ann Endocrinol (Paris) 2001; 62(2): 164–167.
- Quax R.A., Manenschijn L., Koper J.W., Hazes J.M., Lamberts S.W.J., van Rossum E.F.C., Feelders R.A. Glucocorticoid sensitivity in health and disease. Nat Rev Endocrinol 2013; 9(11): 670–686, http://dx.doi.org/10.1038/nrendo.2013.183.
- Barnes P.J. Corticosteroid resistance in patients with asthma and chronic obstructive pulmonary disease. J Allergy Clin Immunol 2013; 131(3): 636–645, http://dx.doi.org/10.1016/j.jaci.2012.12.1564.
- Al-Ramli W., Hamid Q. Th-17 cell-related cytokines’ potential role in the pathogenesis of severe asthma. J Asthma 2008; 45(s1): 41–44, http://dx.doi.org/10.1080/02770900802594759.
- Duan W., Wong W.S. Targeting mitogen-activated protein kinases for asthma. Curr Drug Targets 2006; 7(6): 691–698, http://dx.doi.org/10.2174/138945006777435353.
- Barnes P.J. Theophylline. Am J Respir Crit Care Med 2013; 188(8): 901–906, http://dx.doi.org/10.1164/rccm.201302-0388pp.
- Allen A., Bareille P.J., Rousell V.M. Fluticasone furoate, a novel inhaled corticosteroid, demonstrates prolonged lung absorption kinetics in man compared with inhaled fluticasone propionate. Clin Pharmacokinet 2013; 52(1): 37–42, http://dx.doi.org/10.1007/s40262-012-0021-x.
- Il’ina N.I., Pavlova K.S. Efficacy and safety of Foster in patients with bronchial asthma in real clinical practice. Rossiyskiy allergologicheskiy zhurnal 2010; 5: 82–90.
- Papi A. Inhaled BDP/formoterol extra-fine combination. Evidence and future perspectives. Pneumologie 2009; 63(S 02): S102–S106, http://dx.doi.org/10.1055/s-0029-1214716.
- Papi A., Paggiaro P., Nicolini G., Vignola A.M., Fabbri L.M. Beclomethasone/formoterol vs fluticasone/salmeterol inhaled combination in moderate to severe asthma. Allergy 2007; 62(10): 1182–1188, http://dx.doi.org/10.1111/j.1398-9995.2007.01493.x.
- Pertseva T., Dissanayake S., Kaiser K. Superiority of fluticasone propionate/formoterol fumarate versus fluticasone propionate alone in patients with moderate-to-severe asthma: a randomised controlled trial. Current Curr Med Res Opin 2013; 29(10): 1357–1369, http://dx.doi.org/10.1185/03007995.2013.825592.
- Tan R.A., Corren J. Clinical utility and development of the fluticasone/formoterol combination formulation (Flutiform®) for the treatment of asthma. Drug Des Devel Ther 2014; 8: 1555–1561, http://dx.doi.org/10.2147/dddt.s36556.
- Woodcock A., Bleecker E.R., Lötvall J., O’Byrne P.M., Bateman E.D., Medley H., Ellsworth A., Jacques L., Busse W.W. Efficacy and safety of fluticasone furoate/vilanterol compared with fluticasone propionate/salmeterol combination in adult and adolescent patients with persistent asthma: a randomized trial. Chest 2013; 144(4): 1222–1229, http://dx.doi.org/10.1378/chest.13-0178.
- Berger W.E., Bensch G.W., Weinstein S.F., Skoner D.P., Prenner B.M., Shekar T., Nolte H., Teper A.A. Bronchodilation with mometasone furoate/formoterol fumarate administered by metered-dose inhaler with and without a spacer in children with persistent asthma. Pediatr Pulmonol 2014; 49(5): 441–450, http://dx.doi.org/10.1002/ppul.22850.
- Price D., Kaplan A., Jones R., Freeman D., Burden A., Gould S., von Ziegenweidt J., Ali M., King C., Thomas M. Long-acting muscarinic antagonist use in adults with asthma: real-life prescribing and outcomes of add-on therapy with tiotropium bromide. J Asthma Allergy 2015; 8: 1–13, http://dx.doi.org/10.2147/JAA.S76639.
- Price D., Fromer L., Kaplan A., van der Molen T., Román-Rodríguez M. Is there a rationale and role for long-acting anticholinergic bronchodilators in asthma? NPJ Prim Care Respir Med 2014; 24: 14023, http://dx.doi.org/10.1038/npjpcrm.2014.23.
- Spina D. Current and novel bronchodilators in respiratory disease. Curr Opin Pulm Med 2014; 20(1): 73–86, http://dx.doi.org/10.1097/mcp.0000000000000012.
- Prakash A., Babu K.S., Morjaria J.B. Profile of inhaled glycopyrronium bromide as monotherapy and in fixed-dose combination with indacaterol maleate for the treatment of COPD. Int J Chron Obstruct Pulmon Dis 2015; 10(1): 111–123, http://dx.doi.org/10.2147/copd.s67758.
- Lim H., Nair P. Efficacy and safety of reslizumab in patients with moderate to severe eosinophilic asthma. Expert Rev Respir Med 2015; 9(2): 135–142, http://dx.doi.org/10.1586/17476348.2015.1000867.
- Laviolette M., Gossage D.L., Gauvreau G., Leigh R., Olivenstein R., Katial R., Busse W.W., Wenzel S., Wu Y., Datta V., Kolbeck R., Molfino N.A. Effects of benralizumab on airway eosinophils in asthmatic patients with sputum eosinophilia. J Allergy Clin Immunol 2013; 132(5): 1086–1096, http://dx.doi.org/10.1016/j.jaci.2013.05.020.
- Ortega H.G., Liu M.C., Pavord I.D., Brusselle G.G., FitzGerald J.M., Chetta A., Humbert M., Katz L.E., Keene O.N., Yancey S.W., Chanez P.; MENSA Investigators. Mepolizumab treatment in patients with severe eosinophilic asthma. N Engl J Med 2014; 371(13): 1198–1207, http://dx.doi.org/10.1056/nejmoa1403290.
- Corren J., Lemanske R.F., Hanania N.A., Korenblat P.E., Parsey M.V., Arron J.R., Harris J.M., Scheerens H., Wu L.C., Su Z., Mosesova S., Eisner MD, Bohen S.P., Matthews J.G. Lebrikizumab treatment in adults with asthma. N Engl J Med 2011; 365(12): 1088–1098, http://dx.doi.org/10.1056/NEJMoa1106469.
- Antohe I., Croitoru R., Antoniu S. Tralokinumab for uncontrolled asthma. Expert Opin Biol Ther 2013; 13(2): 323–326, http://dx.doi.org/10.1517/14712598.2012.748740.
- Wenzel S., Ford L., Pearlman D., Spector S., Sher L., Skobieranda F., Wang L., Kirkesseli S., Rocklin R., Bock B., Hamilton J., Ming J.E., Radin A., Stahl N., Yancopoulos G.D., Graham N., Pirozzi G. Dupilumab in persistent asthma with elevated eosinophil levels. N Engl J Med 2013; 368(26): 2455–2466, http://dx.doi.org/10.1056/nejmoa1304048.
- Barnes N., Pavord I., Chuchalin A., Bell J., Hunter M., Lewis T., Parker D., Payton M., Collins L.P., Pettipher R., Steiner J., Perkins C.M. A randomized, double-blind, placebo-controlled study of the CRTH2 antagonist OC000459 in moderate persistent asthma. Clin Exp Allergy 2012; 42(1): 38–48, http://dx.doi.org/10.1111/j.1365-2222.2011.03813.x.
- Pettipher R., Hunter M.G., Perkins C.M., Collins L.P., Lewis T., Baillet M., Steiner J., Bell J., Payton M.A. Heightened response of eosinophilic asthmatic patients to the CRTH2 antagonist OC000459. Allergy 2014; 69(9): 1223–1232, http://dx.doi.org/10.1111/all.12451.
- Bateman E.D., Kornmann O., Schmidt P., Pivovarova A., Engel M., Fabbri L.M. Tiotropium is noninferior to salmeterol in maintaining improved lung function in B16-Arg/Arg patients with asthma. J Allergy Clin Immunol 2011; 128(2): 315–322, http://dx.doi.org/10.1016/j.jaci.2011.06.004.
- Kerstjens H.A.M., Disse B., Schröder-Babo W., Bantje T.A., Gahlemann M., Sigmund R., Engel M., van Noord J.A. Tiotropium improves lung function in patients with severe uncontrolled asthma: a randomized controlled trial. J Allergy Clin Immunol 2011; 128(2): 308–314, http://dx.doi.org/10.1016/j.jaci.2011.04.039.
- Kerstjens H.A.M., Engel M., Dahl R., Paggiaro P., Beck E., Vandewalker M., Sigmund R., Seibold W., Moroni-Zentgraf P., Bateman E.D. Tiotropium in asthma poorly controlled with standard combination therapy. N Engl J Med 2012 Sep 27; 367(13): 1198–11207, http://dx.doi.org/10.1056/nejmoa1208606.
- Balabolkin I.I., Smirnov I.E., Lyapunov A.A., Lukina F., Goryunov A.V., Goncharova N.V., Reutova V.S. Montelukast therapy efficacy in children with bronchial asthma. Voprosy sovremennoy pediatrii 2006; 5(5): 35–39.
- Ciółkowski J., Mazurek H., Stasiowska B. Evaluation of step-down therapy from an inhaled steroid to montelukast in childhood asthma. Allergol Immunopathol (Madr) 2014; 42(4): 282–228, http://dx.doi.org/10.1016/j.aller.2013.01.005.
- Bush A. Montelukast in paediatric asthma: where we are now and what still needs to be done? Paediatr Respir Rev 2015; 16(2): 97–100, http://dx.doi.org/10.1016/j.prrv.2014.10.007.
- Gauvreau G.M., Boulet L.-P., Schmid-Wirlitsch C., Côté J., Duong M., Killian K.J., Milot J., Deschesnes F., Strinich T., Watson R.M., Bredenbröker D., O’Byrne P.M. Roflumilast attenuates allergen-induced inflammation in mild asthmatic subjects. Respir Res 2011; 12(1): 140, http://dx.doi.org/10.1186/1465-9921-12-140.
- Geppe N.A., Ozerskaya I.V. Role of cromones in bronchial asthma and allergic rhinitis therapy in children. Atmosfera. Pul’monologiya i allergologiya 2009; 1: 11–14.
- Howrylak J.A., Fuhlbrigge A.L., Strunk R.C., Zeiger R.S., Weiss S.T., Raby B.A. Classification of childhood asthma phenotypes and long-term clinical responses to inhaled anti-inflammatory medications. J Allergy Clin Immunol 2014; 133(5): 1286–1300, http://dx.doi.org/10.1016/j.jaci.2014.02.006.
- Netzer N.C., Küpper T., Voss H.W., Eliasson A.H. The actual role of sodium cromoglycate in the treatment of asthma: a critical review. Sleep Breath 2012; 16(4): 1027–1032, http://dx.doi.org/10.1007/s11325-011-0639-1.
- Vishneva E.A., Namazova-Baranova L.S., Alekseeva A.A., Efendieva K.E., Levina Yu.G., Voznesenskaya N.I., Tomilova A.Yu., Selimzyanova L.R., Promyslova E.A. Children asthma: key principles of obtaining control in recent times. Pediatricheskaya farmakologiya 2013; 10(4): 60–72.
- Tsyplenkova S.E., Mizernitsky Yu.L., Sokolova L.V., Sorokina E.V. New opportunities of monitoring the efficiency of anti-IgE therapy for severe asthma in childrens. Rossiyskiy vestnik perinatologii i pediatrii 2012; 3: 47–52.
- Hanania N.A., Alpan O., Hamilos D.L., Condemi J.J., Reyes-Rivera I., Zhu J., Rosen K.E., Eisner MD, Wong D.A., Busse W. Omalizumab in severe allergic asthma inadequately controlled with standard therapy: a randomized trial. Ann Intern Med 2011; 154(9): 573–582, http://dx.doi.org/10.7326/0003-4819-154-9-201105030-00002.
- Giovannini-Chami L., Albertini M., Scheinmann P., de Blic J. New insights into the treatment of severe asthma in children. Paediatr Respir Rev 2014, http://dx.doi.org/10.1016/j.prrv.2014.07.006.
- Pajno G.B., Nadeau K.C., Passalacqua G., Caminiti L., Hobson B., Jay D.C., Arasi S., Chiera F., Salzano G. The evolution of allergen and non-specific immunotherapy: past achievements, current applications and future outlook. Expert Review of Clinical Immunology 2015; 11(1): 141–154, http://dx.doi.org/10.1586/1744666X.2015.977260.
- Pavord I.D., Korn S., Howarth P., Bleecker E.R., Buhl R., Keene O.N., Ortega H., Chanez P. Mepolizumab for severe eosinophilic asthma (DREAM): a multicentre, double-blind, placebo-controlled trial. Lancet 2012; 380(9842): 651–659, http://dx.doi.org/10.1016/s0140-6736(12)60988-x.
- Grunig G., Warnock M., Wakil A.E., Venkayya R., Brombacher F., Rennick D.M., Sheppard D., Mohrs M., Donaldson D.D., Locksley R.M., Corry D.B. Requirement for IL-13 independently of IL-4 in experimental asthma. Science 1998; 282(5397): 2261–2263, http://dx.doi.org/10.1126/science.282.5397.2261.
- Sidhu S.S., Yuan S., Innes A.L., Kerr S., Woodruff P.G., Hou L., Muller S.J., Fahy J.V. Roles of epithelial cell-derived periostin in TGF-beta activation, collagen production, and collagen gel elasticity in asthma. Proc Natl Acad Sci USA 2010; 107(32): 14170–1475, http://dx.doi.org/10.1073/pnas.1009426107.
- Masuoka M., Shiraishi H., Ohta S., Suzuki S., Arima K., Aoki S., Toda S., Inagaki N., Kurihara Y., Hayashida S., Takeuchi S., Koike K., Ono J., Noshiro H., Furue M., Conway S.J., Narisawa Y., Izuhara K. Periostin promotes chronic allergic inflammation in response to Th2 cytokines. J Clin Invest 2012; 122(7): 2590–2600, http://dx.doi.org/10.1172/JCI58978.
- Giovannini-Chami L., Marcet B., Moreilhon C., Chevalier B., Illie M.I., Lebrigand K., Robbe-Sermesant K., Bourrier T., Michiels J.F., Mari B., Crénesse D., Hofman P., de Blic J., Castillo L., Albertini M., Barbry P. Distinct epithelial gene expression phenotypes in childhood respiratory allergy. Eur Respir J 2012; 39(5): 1197–1205, http://dx.doi.org/10.1183/09031936.00070511.
- Castro M., Mathur S., Hargreave F., Boulet L.P., Xie F., Young J., Wilkins H.J., Henkel T., Nair P.; Res-5-0010 Study Group. Reslizumab for poorly controlled, eosinophilic asthma: a randomized, placebo-controlled study. Am J Respir Crit Care Med 2011; 184(10): 1125–1132, http://dx.doi.org/10.1164/rccm.201103-0396oc.
- Borish L.C., Nelson H.S., Lanz M.J., Claussen L., Whitmore J.B., Agosti J.M., Garrison L. Interleukin-4 receptor in moderate atopic asthma. A phase I/II randomized, placebo-controlled trial. Am J Respir Crit Care Med 1999; 160(6): 1816–1823, http://dx.doi.org/10.1164/ajrccm.160.6.9808146.
- Getz E.B., Fisher D.M., Fuller R. Human pharmacokinetics/pharmacodynamics of an interleukin-4 and interleukin-13 dual antagonist in asthma. J Clin Pharmacol 2009; 49(9): 1025–1036, http://dx.doi.org/10.1177/0091270009341183.
- Wenzel S., Wilbraham D., Fuller R., Getz E.B., Longphre M. Effect of an interleukin-4 variant on late phase asthmatic response to allergen challenge in asthmatic patients: results of two phase 2a studies. Lancet 2007; 370(9596): 1422–1431, http://dx.doi.org/10.1016/s0140-6736(07)61600-6.
- Corren J., Busse W., Meltzer E.O., Mansfield L., Bensch G., Fahrenholz J., Wenzel S.E., Chon Y., Dunn M., Weng H.H., Lin S.L. A randomized, controlled, phase 2 study of AMG 317, an IL-4Ralpha antagonist, in patients with asthma. Am J Respir Crit Care Med 2010; 181(8): 788–796, http://dx.doi.org/10.1164/rccm.200909-1448oc.
- Parker J.M., Oh C.K., LaForce C., Miller S.D., Pearlman D.S., Le C., Robbie G.J., White W.I., White B., Molfino N.A.; MEDI-528 Clinical Trials Group. Safety profile and clinical activity of multiple subcutaneous doses of MEDI-528, a humanized anti-interleukin-9 monoclonal antibody, in two randomized phase 2a studies in subjects with asthma. BMC Pulm Med 2011; 11: 14, http://dx.doi.org/10.1186/1471-2466-11-14.
- Gauvreau G.M., O’Byrne P.M., Boulet L.P., Wang Y., Cockcroft D., Bigler J., FitzGerald J.M., Boedigheimer M., Davis B.E., Dias C., Gorski K.S., Smith L., Bautista E., Comeau M.R., Leigh R., Parnes J.R. Effects of an anti-TSLP antibody on allergen-induced asthmatic responses. N Engl J Med 2014; 2102–2110, http://dx.doi.org/10.1056/nejmoa1402895.
- Reichert J.M. Antibodies to watch in 2015. MAbs 2015; 7(1): 1–8, http://dx.doi.org/10.4161/19420862.2015.988944.
- Demko I.V., Sobko E.A., Ishenko O.P., Solov’eva V.A. Clinical efficiency of specific immunotherapy in bronchial asthma. Sibirskoe meditsinskoe obozrenie 2010; 62(2): 72–76.
- Balabolkin I.I., Ryleeva I.V., Yukhtina N.V., Ksenzova L.D., Kapustina E.Yu. Allergen-specific immune therapy in children with allergic diseases and possibilities of efficiency improvement. Pediatriya 2006; 2: 81–85.
- Balabolkin I.I., Bulgakova V.A., Sedova M.S., Sentsova T.B. Allergen-specific immune therapy in children with bronchial asthma and frequent acute respiratory infections. Allergologiya i immunologiya 2007; 8: 116.
- Eliseeva Т.I., Knyazeva Е.V., Bochkova Y.S., Kononova S.V., Geppe N.A., Balabolkin I.I. Spirographic parameters and their change in bronchial patency variability tests in control level assessment of bronchial asthma in children. Sovremennye tehnologii v medicine 2013; 5(4): 94–101.